
What is Vascular Ehlers-Danlos syndrome (VEDS)?
Vascular Ehlers-Danlos syndrome (VEDS) is a genetic condition that is caused by a change (mutation) in the gene for collagen type 3 (the COL3A1 gene). This mutation may come from a parent with the syndrome or be due to a new change in the gene. VEDS is autosomal dominant, which means that if a parent has the condition, there is a 50% chance each child will have the condition. Collagens are part of our body’s connective tissue. Collagens play an important role in the structure and function of bones, muscles, skin, tendons, organs, and blood vessels. People with VEDS have abnormal function of type 3 collagen and may have a wide range of features that range from spontaneous and easy bruising with little or no change in lifespan to bowel and/or arterial and aortic rupture or dissection at a young age and a reduced lifespan. Women with VEDS have the potential of a rupture of the uterus during pregnancy that may substantially shorten lifespan. Some people with VEDS have a characteristic facial appearance (Figure 1), thin skin, and tissue fragility that could indicate the condition is present and assist in recognition of the condition before there is a major complication.

How common is VEDS?
The exact number of people with VEDS is not known, although it is estimated at 1 in 50,000 to 1 in 100,000 people. We think there are between 6,000 and 8,000 people in the U.S. with VEDS.
What are the features of VEDS?
It is important to remember that the features of VEDS can be highly variable and that a high level of suspicion is necessary to consider this diagnosis. The first presentation of VEDS may be life-threatening, such as an arterial rupture, arterial dissection, or organ rupture. The presence of one major feature of VEDS, especially in a young person, should prompt further evaluation for VEDS. The presence of multiple minor features, with or without a major feature, warrants further evaluation.
The major features are:
- Family history of VEDS
- Artery rupture (burst artery) or dissection (tear) at a young age
- Rupture of the intestine that is not caused by a known issue
- Rupture of the uterus during the third trimester of pregnancy. This is not a result of previous c-section
- Severe vaginal tears during sex or childbirth
- Arteriovenous carotid-cavernous sinus fistula (which can present with sudden redness and enlargement of the eye not caused by trauma)
The minor features are:
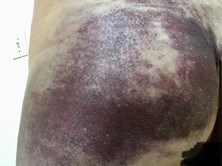
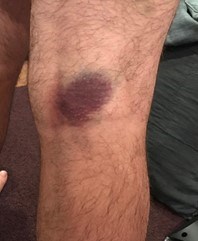
- Easy bruising (Figure 2)
- Bruising in unusual sites, such as cheeks and back
- Thin, translucent skin with veins that are clearly seen
- Thin lips, small chin, thin nose, large, deep-set eyes (Figure 1)
- Collapse of the lung leading to air in the lung cavity (called pneumothorax)
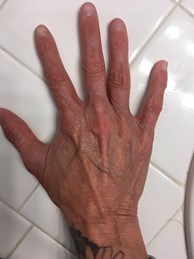
- Hands and fingers look like those of a much older person (called acrogeria) (Figures 3-4)
- Clubfoot (talipes equinovarus)
- Dislocated hip at birth
- Small joints that can bend more than the expected amount
- Tendon/muscle rupture
- Varicose veins before the age of 30
- Recurrent pneumothorax
What testing is needed?
To diagnose VEDS, a doctor must review an individual’s medical and family history. They will also look to see if the person has any physical features of VEDS. If the evaluation raises the concern that the individual may have VEDS, a DNA test can confirm the COL3A1 mutation that causes this condition.
How is VEDS treated?
It is recommended that people with VEDS:
- Establish a care team of doctors to make sure they get the best care. These doctors should include:
- A vascular medicine doctor or cardiologist
- Vascular surgeon
- General surgeon
- Geneticist
- The cooperation among these doctors should create emergency preparedness and assurance that ordinary care proceeds. It is important to find a doctor who is knowledgeable about VEDS.
- Have ongoing monitoring. Individuals with VEDS should get an annual physical examination and discuss any signs or symptoms of concern. Many specialists recommend routine and serial monitoring of the entire vascular tree (from the head to the pelvis) to detect abnormalities of the blood vessels, even before any symptoms develop. However, the evidence for this approach is weak. If a person has known artery problems (such as an aneurysm or arterial dissection), they should have imaging every six to 12 months. This imaging should be done by ultrasound, computerized tomography angiography (CTA), or magnetic resonance angiography (MRA) and will be used to see when treatment is needed.
- Follow doctors’ medication recommendations. If a person has high blood pressure (hypertension), it is important they take blood pressure medication to keep their blood pressure low. Even in the absence of high blood pressure, many experts recommend treatment with a beta blocker. Beta blockers may lessen the stress on blood vessel walls. Celiprolol is a beta blocker available in Europe and may decrease problems with the arteries and improve outcomes, although the evidence demonstrating effectiveness of celiprolol to improve outcomes is debated. There have not been any studies of other beta blockers in VEDS, so we do not know whether other beta blockers (such as nebivolol, carvedilol, atenolol, or metoprolol) are effective. Treatment may also include pain medication for joints and muscles.
- Have surgery when recommended by their doctor and surgeon. Surgical procedures are best done by a surgeon and anesthesiologist who know about VEDS and have experience with operating on fragile tissues. In some cases, surgery on blood vessels or damaged joints may be necessary before an emergency occurs. This is preferable to emergency surgery. Because blood vessels and other hollow organs are fragile and subject to rupture in people with VEDS, doctors recommend surgery only when there is a risk of life-threatening bleeding.
- Individuals with VEDS may benefit from seeing a physical therapist to strengthen their muscles. A physical or occupational therapist with knowledge about VEDS can offer safe exercises.
- When someone is diagnosed with VEDS, their doctor may recommend imaging of the blood vessels from head to pelvis and sometimes the upper legs. This will be done with a CT angiogram or an MR angiogram. They will also have an echocardiogram to evaluate the heart and valves. If these tests are normal, they will need to go back for regular appointments, including:
- History and physical exam – every year
- Repeat imaging – every two years. This may be done more often if problems with the blood vessels are seen.
- In general, routine invasive screening tests, such as a colonoscopy, are not performed in VEDS unless the benefits outweigh the risks. Arteriography (an invasive test requiring inserting a catheter into a blood vessel) carries a higher risk of trauma, bleeding, and rupture of the artery in VEDS. Individuals with VEDS should talk to their doctor about whether they should get a colonoscopy or arteriography. These can be more dangerous in people with VEDS.
- Avoid constipation. Constipation increases the risk for bowel perforation, a life-threatening complication associated with VEDS. Many people with VEDS benefit from a regular stool softener and laxative regimen. When using laxatives, it is generally recommended to avoid stimulant laxatives that cause the bowels to contract, and favor laxatives that work by drawing fluid into the bowels (such as MiraLAX©).
Are there limitations on exercise?
People with VEDS should avoid circumstances that can cause medical problems, such as contact sports, heavy lifting, intense weight training, and activities that may include sudden impact or jarring of the body.
Exercise should be modified according to a doctor’s recommendations. Children with VEDS may need a modified exercise plan at school. It is essential to discuss physical activities and specific activity levels with a knowledgeable physician so that exercise can be incorporated safely into the regular healthcare routine. This should be an ongoing conversation because, as children age, their medical status and desires can change. Anyone with VEDS should favor a non-competitive activity performed at a pace that permits conversation, such as brisk walking, leisurely bicycling, slow jogging, shooting baskets, leisurely tennis or swimming, and use of light weights without straining.
Some children with mild forms of VEDS have been successful in competitive environments in non-collision sports.
How does VEDS affect one’s ability to start a family?
Pregnancy carries an increased risk of complications in women with VEDS. It is very important to have an informed discussion with a VEDS medical team before contemplating pregnancy. Pregnancy risk includes life-threatening complications such as arterial dissection and rupture, uterine rupture, and surgical complications as well as preterm delivery, lacerations, and poor wound healing. Pregnant women with VEDS should be followed by a high-risk maternal-fetal specialist. The type of COL3A1 mutation present may provide prognostic information about the natural history of the condition and may impact maternal risks of pregnancy. A recent study from the University of Washington reported a pregnancy-related death rate of about 5% per delivery, with all fatalities occurring in women with protein-altering mutations. However, there were no deaths reported among the subgroup of women with null mutations in COL3A1.
Prenatal testing is available for pregnancies because of a known disease-causing mutation in one of the parents. Genetic counseling is an important aspect of care and generally includes discussions prior to becoming pregnant. Pre-implantation genetic diagnosis, in which unaffected embryos are selected for implantation, can eliminate the risk of transmission from an affected parent.
In addition to careful assessment of the risk for women contemplating pregnancies, couples in whom the underlying genetic defect is known may consider prenatal or pre-implantation diagnostics.
- Prenatal testing
- Prenatal testing is the technique in which early in the pregnancy (11-12 weeks) the presence of the genetic defect is checked by means of a so-called villous sampling in which a piece of placenta (which is of fetal origin) is punctured away. If the result is abnormal, the pregnancy will be ended. With this technique, pregnancy occurs naturally but there is a 50% chance that the pregnancy must be ended.
- Pre-gestational diagnostic (PGD)
- PGD is a technique that was developed more recently and where embryos are developed via an in vitro fertilization procedure. For this, oocytes are removed from the ovaries after stimulation and are fertilized with sperm in a test tube. In an early stage of embryo development, one cell is subsequently removed for testing for the presence of the genetic defect. Only non-affected embryos are replaced. With this technique, the pregnancy is artificially established.
In both cases, knowledge of the pathogenic variant gene change is an absolute requirement. Couples must also have dedicated pre-conceptual counseling. Experience with use of assisted reproductive technologies for women with VEDS is limited.
The method of delivery for women with VEDS may include assisted vaginal delivery with epidural anesthesia, methods to avoid pushing and straining, or cesarean section. There are not adequate data to recommend one type of delivery method over the other. Shared decision making by a knowledgeable team (including cardiologist/vascular specialist/maternal fetal medicine/anesthesia) is recommended.
What are the signs of an acute aortic event? What should be done if one occurs?
Everyone with VEDS should wear an identifying medical alert bracelet or necklace and carry an information card for emergency care.
Prepare in advance for a potential emergency. VEDS is considered the most serious form of Ehlers-Danlos syndrome due to the possibility of arterial or organ rupture. If someone with VEDS experiences sudden or severe headache, neck, chest, abdominal, or extremity pain or bleeding, they should go to a hospital emergency department immediately. Tests, such as MRA, MRI, and CT, can identify arterial or bowel complications, such as a rupture, that require surgery or problems like a collapsed lung (pneumothorax). Individuals should have emergency instructions from their personal physician to provide EMS workers in case of emergency. Families should also be proactive and alert local first responders to their diagnosis.
A medical alert bracelet can alert emergency personnel right away that someone is at risk for a life-threatening event. Medical alert bracelets are available at no cost to individuals with a genetically confirmed diagnosis of VEDS. Click here for more information.
Where can I learn more about VEDS?
The VEDS Movement, a division of The Marfan Foundation: https://www.thevedsmovement.org
VEDS Collaborative: https://www.vedscollaborative.org/
Get the latest news on genetic aortic and vascular conditions
If you have an interest in advancing the research, education, and treatment of genetic aortic and vascular conditions, sign up for emails from the GenTAC Alliance using the form to the right.
These communications are geared toward professionals and include information such as updates to best practices and treatment guidelines, upcoming scientific and clinical webinars, and newly developed tools for healthcare professionals and researchers.
Join the GenTAC Alliance Mailing List
